Cutaneous Nocardia brasiliensis Infection in an Immunocompetent Patient
Alexandre G Lellouch, Lior Amsallem, Zhi Yang Ng and Nicolas Robert
DOI10.4172/2472-1905.100024
1Division of Plastic and Reconstructive Surgery, Massachusetts General Hospital, Harvard Medical School, Boston, MA, USA
2Vascularized Composite Allotransplantation Laboratory, Center for Transplantation Sciences, Massachusetts General Hospital, Boston, MA, USA
3Hand Surgery Department, Saint Antoine Hospital, 75012 Paris, France
- *Corresponding Author:
- Alexandre G Lellouch
HandSurgery Department
Saint Antoine Hospital, 75012 Paris
France.
Tel: 9141245548
Fax: 6177264067
E-mail: lellouchalexandre@gmail.com
Received date: December 12, 2016; Accepted date: January 11, 2017; Published date: January 20, 2017
Citation: Lellouch AG, Amsallem L, Ng ZY, et al. Cutaneous Nocardia brasiliensis Infection in an Immunocompetent Patient. J Aesthet Reconstr Surg. 2017, 3:1. doi: 10.4172/2472-1905.100024
Abstract
Nocardia Brasiliensis infections involving the hand are uncommon. Optimal treatment involves a combination of surgical debridement and appropriate antimicrobial therapy. However, identification of this pathogen is usually delayed and the lack of timely may compromise on functional outcomes.
Keywords
Nocardia brasiliensis; Immunocompetent; Adenophlegmon; Lymphangitis
Introduction
In the field of hand surgery, phlegmon is a common emergency. Microbiological sampling during surgical treatment is recommended with staphylococcus and streptococcus commonly identified [1]. In most cases, broad-spectrum intravenous antibiotic therapy is required in the postoperative phase [2,3]. However, some pathogens require specific antibiotic treatment. We report here a rare case of Nocardia brasiliensis infection of the hand in an immunocompetent elderly patient.
Case Study
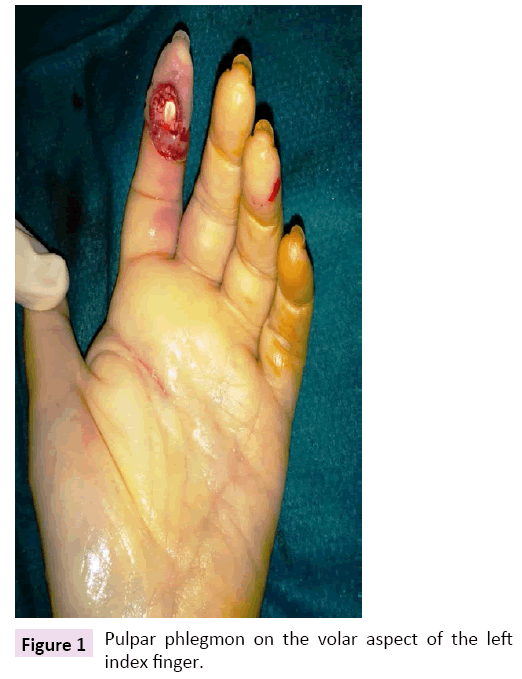
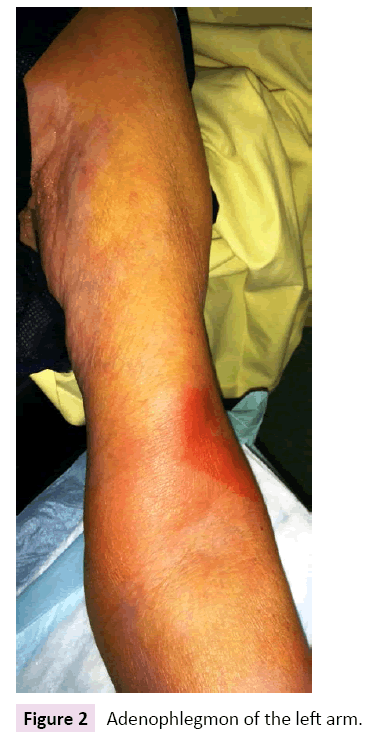
A 72-year-old French woman presented to the emergency department with an infection of the left index finger. Her past medical history was significant for bipolar disorder for which she is on valproate, oxazepam and zopiclone. She had previously been seen two days ago by her general practitioner who prescribed amoxicillin+clavulanic acid. Clinical examination revealed a pulpar phlegmon on the left index (Figure 1) with pain along the flexor sheath, ascending lymphangitis and an adenophlegmon in the antecubital fossa (Figure 2). Standard hand X-rays did not reveal any osteitis or foreign body. On further questioning, the patient denied preceding trauma and infections. She lived alone, did not do any gardening and had not travelled within the past year.
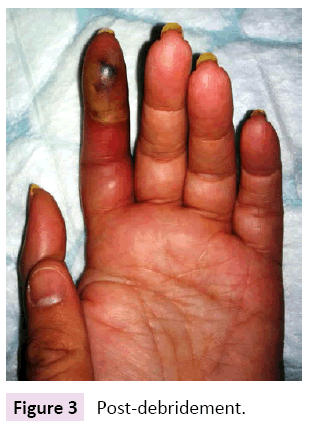
The patient was then transferred to the operating room for definitive surgical treatment under loco-regional anesthesia: necrotic tissue of the pulpar phlegmon was excised (Figure 3) and a counter incision was performed for anterograde cleansing and drainage of the flexor sheath, and synovectomy of the adenophlegmon. Frank pus was found and samples were taken for microbiology. Due to regional extension of the infection, empiric antibiotic coverage with IV amoxicillin+clavulanic acid was initiated. Cultures were positive for N. brasiliensis (Table 1) and a three-month course of PO cotrimoxazole was started. In view of the bacterial isolate, further workup with staging scans were done (CT chest/abdomen/pelvis, CXR) as well as immunologic assessment (HIV serology, fasting blood sugar, protein electrophoresis); all test results returned negative. The patient’s recovery was otherwise unremarkable and no septic recurrence was observed after completing antibiotic treatment.
| ANTIBIOGRAM: Nocardia Brasiliensis | |
|---|---|
| R: Ampicillin | S: Gentamycin |
| S: Amoxycilin | S: Tobramycin |
| S: Amoxycilin+Clavulanic acid | S: Amikacin |
| S: Ticarcillin+Clavulanic acid | S: Minocycline |
| S: Piperacillin+Tazobactum | R: Doxycycline |
| R: Imipenem | S: Tigecycline |
| R: Meropenem | R: Erythromycin |
| R: Ertapenem | S: Linezolid |
| R: Doripenem | R: Vancomycin |
| S: Cefuroxime | R: Trimethoprim |
| S: Cefotaxime | S: Trimethoprim+sulfamethoxazole |
| S: Ceftriaxone | R: Ciprofloxacine |
| S: Cefepime | S: Levoflaxacin |
| R: Pristinamycin | R: Rifampicin |
Table 1: Antibiogram.
N. brasiliensis has been found in the soil in many tropical and subtropical areas but rarely in temperate regions. Diagnosis is challenging because the clinical picture is non-specific [4,5] and presents in various forms: Primary cutaneous (superficial skin infection), subcutaneous abscess [6], pyoderma [6], ulceration [6], cellulitis [6], lymphangitis, mycetoma (chronic form) and even necrotizing cutaneous tissue [7]. Nevertheless, some clinical signs are highly suggestive such as nodular lymphangitis [8,9]. Typically, traumatic inoculation of N. brasiliensis into the skin develops into an infection in immunocompetent hosts, resulting in acute inflammatory responses as depicted in our case. The optimal treatment strategy for cutaneous N. brasiliensis infection is a combination of surgical excision and pus drainage together with cotrimoxazole antibiotic therapy. The duration of antibiotic treatment is not well-defined, but current evidence suggests that it must be sufficient to allow complete eradication especially in immunocompetent patients [4,10-12].
In cases with hand involvement, should clinical improvement not be achieved following surgery and empirical IV antibiotics, further surgery and early initiation of cotrimoxazole may be required prior to identification of the pathogen. Indeed, clinical recognition of the possibility of N. brasiliensis infections by hand surgeons is essential to prevent delay in appropriate treatment and the attendant sequelae including permanent hand stiffness. According to the literature, typical penicillin-based, broadspectrum antibiotics are inappropriate for the treatment of N. brasiliensis infections in most cases [10].
Conclusion
Acute N. brasiliensis phlegmon is uncommon but has to be suspected in cases associated with adenophlegmon in the ipsilateral limb. Cotrimoxazole antibiotic therapy has to be of at least 6 weeks’ duration [13,14] to allow sufficient eradication. Additional work-up during the time of presentation should also be performed to evaluate for possible underlying etiologies that may contribute towards an immunocompromised state.
Acknowledgement
There is no conflict of interest. Verbal consent was obtained from the patient.
References
- Carmes S, Tekam A, Rogier A, Brouste Y, Dumontier C (2011) Epidemiologie des panaris de la pulpe. Chir Main 30: 428
- Delgrande D, Pierrart J, Mamane W, et al. (2014) Panaris et antibiotherapie post operatoire : evaluation des pratiques. Chir Main 33: 420
- Delgrande D, Pierrart J, Mamane W, et al. (2014) Inutilite des antibiotiques en postoperatoire dans la prise en charge des panaris : serie prospective de 46 cas. Chir Main 33: 420
- Dodiuk-Gad R, Cohen E, Ziv M, et al. (2010) Cutaneousnocardiosis : report of two cases and review of the literature. Int J dermatol 49: 1380-1385
- Schall K, Lee H. (1992) Actinomycete infections in humans: areview. Gene 115: 201-211
- Tara Lykowski A, Emil orpilla R, Richard Hayek J (2008) The historyholds the key in thisgardenerwith a skin infection. JAAPA 21: 35-7
- Joseph Ricci A, Ana Weil A, Kyle Eberlin R (2015) NecrotizingcutaneousNocardiosis of the Hand: A case report. J Hand Microsurg 7: 224-7
- Sharma NL, Mahajan VK, Agarwal S, Katoch VM (2008) Nocardialmycetoma: Diverse clinicalpresentations. Indian J Dermatol, Venereology and Leprology 74: 635-640
- Jorn Andreas Lohmeyer, Hans Günther Machens, Klaus Dieter Werber (2010) A case of severecutaneousnocardiosis. J Hand SurgEur 35: 72-3
- Smego R, Moeller M, Gallis H (1983) Trimethoprim-sulfamethoxazoletherapy for Nocardia infections. ArchIntern Med 143: 711-718
- Burgert SJ (1999) Nocardiosis: aclinicalreview. Inf Dis Clin Pract 8: 27-32
- Shifren JD, Milliken RG (1996) An acute Nocardiabrasiliensis Infection of the Hand: a case report. J Hand Surg Am 21: 309-310
- Kalb RE, Kaplan MH, Grossman ME (1985) Cutaneousnocardiosis. Case reports and review. J Am AcadDermatol 13: 125-33
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences